Joseph made clear in its announcement that abandonment of the trauma network was accelerated by Gov. The response from public officials has not been helpful. At the Huntington, for example, 15% of all patients are Medi-Cal. Hospital budgets already are heavily affected by their Medi-Cal contracts, which pay less than 70% of the actual costs of treatment. Probably most of the intensive-care unit and acute-care hospital costs for trauma patients go unpaid, adding to the burden of private hospitals for indigent patients they cannot transfer to a county facility.įurthermore, the hospitals are required to pay the county a $35,000 fee to cover costs of a computer information network that analyzes trauma services and costs. And the costs do not stop at the trauma center. Hospitals also must pay the high cost of malpractice insurance for the trauma doctors. 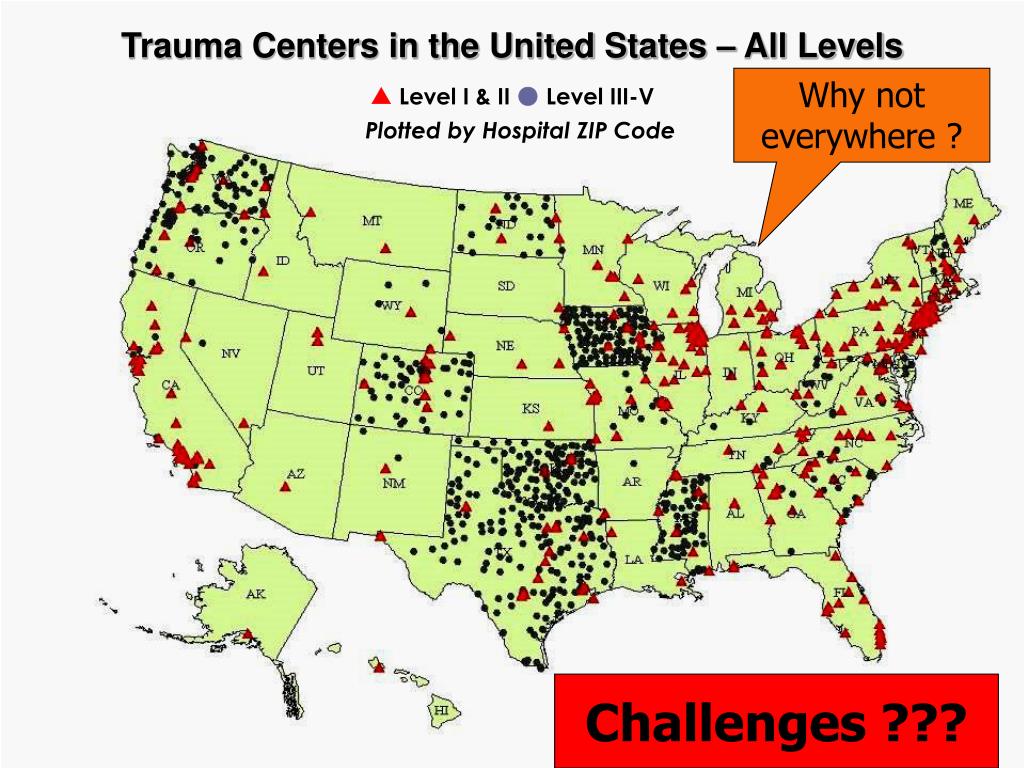 
Understandably, they are now insisting on compensation for standing by. But the standby specialists, including neurosurgeons and orthopedic surgeons, who initially volunteered, also are part of the cost. It is the instant availability and schooled teamwork of those staffs that set trauma centers apart from emergency rooms. Trauma centers have high direct costs, because they must maintain trauma surgeons and anesthesiologists on duty at all times. The Huntington intensive care units were at saturation seven times in January. Furthermore, both Northridge and Huntington have recently had more periods when they could accept no additional trauma patients because of saturation in their intensive-care units. All of them have under regular review their ability to continue. Each of the three trauma centers that will be affected by the closing-Northridge, Holy Cross Medical Center in Mission Hills and Huntington in Pasadena-already are sustaining annual trauma-generated losses of $1 million to $1.8 million. 
Joseph estimates that it lost almost $2 million last year as a result of the trauma operation. John McConnellogue, medical director of the trauma operation at the Northridge Hospital Medical Center. “The majority of the patients are people like you and me, driving a freeway,” said Dr. But the trauma network deterioration has a special meaning, because it affects the safety of everyone, rich and poor, who travel the freeways and highways of the region: 65% of the trauma cases are traffic-related. Indeed, it is a money issue, part of a broader problem of an unraveling health-safety net that goes beyond trauma centers and includes the whole issue of uncompensated and undercompensated hospital and medical care, and the 5.2 million Californians and 37 million Americans who have no health insurance. “The problem is, where is it coming from?” Gaspard, medical director of the trauma center at Huntington Memorial Hospital in Pasadena. Joseph Medical Center in Burbank, the county will have lost nine of the 23 trauma centers established in 1983. With the closing June 19 of the trauma center at St. The deprived areas in Eastern San Gabriel Valley and around the Los Angeles International Airport soon will spread to Eastern San Fernando Valley. A map in the Trauma Hospital Program office of the Los Angeles County Department of Health Services charts the deterioration of the trauma network, with areas of crosshatching marking the regions no longer within 20 minutes by ambulance from a trauma center.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
